Abstract
Purpose
The aim of the study was to evaluate the incidence and type of actual drug–drug interactions (DDIs) that result in adverse drug reactions (ADRs) or diminished therapeutic effect in elderly patients within 30 days of discharge from an internal medicine clinic.
Methods
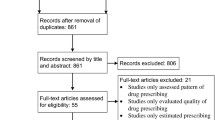
A prospective observational study was conducted at the Internal Medicine Clinic of University Hospital Dubrava, Zagreb, Croatia, between October and December 2011. Patients aged ≥65 years discharged from the Internal Medicine Clinic during the study period with a prescription for two or more medications were eligible for inclusion in the study. A total of 222 patients were ultimately enrolled in the study. For each patient, potential DDIs were identified using Lexi-Interact software. The follow-up visit was scheduled approximately 30 days after discharge. Causality between DDIs and ADRs or diminished therapeutic effect of drugs was assessed by two independent clinicians.
Results
Potential DDIs were identified in 190 (85.6 %) patients. Actual DDIs were detected in 21 (9.5 %) patients. In 19 patients, DDIs resulted in an ADR. Diminished therapeutic effect resulting from DDIs was detected in two patients. Angiotensin-converting enzyme inhibitors were the drug class most frequently associated with DDI-related ADRs.
Conclusions
A significant incidence of actual DDIs suggests that DDIs play an important role in patient safety. Drug therapy should be initiated if absolutely necessary, and the number of drugs used to treat elderly patients should be minimized to reduce the incidence of DDI-related adverse patient outcomes.
Similar content being viewed by others
References
Hartshorn EA (2006) Drug interaction: 1. General considerations. Ann Pharmacother 40:116–118
Hines LE, Murphy JE (2011) Potentially harmful drug–drug interactions in the elderly: a review. Am J Geriatr Pharmacother 9:364–377. doi:10.1016/j.amjopharm.2011.10.004
Mallet L, Spinewine A, Huang A (2007) The challenge of managing drug interactions in elderly people. Lancet 370:185–191
Delafuente JC (2003) Understanding and preventing drug interactions in elderly patients. Crit Rev Oncol Hematol 48:133–143
Björkman IK, Fastbom J, Schmidt IK, Bernsten CB, Pharmaceutical Care of the Elderly in Europe Research (PEER) Group (2002) Drug–drug interactions in the elderly. Ann Pharmacother 36:1675–1681
Becker ML, Kallewaard M, Caspers PW, Visser LE, Leufkens HG, Stricker BH (2007) Hospitalisations and emergency department visits due to drug–drug interactions: a literature review. Pharmacoepidemiol Drug Saf 16:641–651
Becker ML, Visser LE, van Gelder T, Hofman A, Stricker BH (2008) Increasing exposure to drug–drug interactions between 1992 and 2005 in people aged ≥55 years. Drugs Aging 25:145–152
Magro L, Moretti U, Leone R (2012) Epidemiology and characteristics of adverse drug reactions caused by drug–drug interactions. Expert Opin Drug Saf 11:83–94
Mirosevic Skvrce N, Macolic Sarinic V, Mucalo I, Krnic D, Bozina N, Tomic S (2011) Adverse drug reactions caused by drug-drug interactions reported to Croatian Agency for Medicinal Products and Medical Devices: a retrospective observational study. Croat Med J 52:604–614
Seymour RM, Routledge PA (1998) Important drug–drug interactions in the elderly. Drugs Aging 12:485–494
Gagne JJ, Maio V, Rabinowitz C (2008) Prevalence and predictors of potential drug-drug interactions in Regione Emilia-Romagna, Italy. J Clin Pharm Ther 33:141–151
Lexi-Comp Online (2012) Lexi-Interact. Wolters Kluwer Health Clinical Solutions, Minneapolis. Available at: http://online.lexi.com/lco/action/interact. Accessed 3 Aug 2012
Naranjo CA, Busto U, Sellers EM, Sandor P, Ruiz I, Roberts EA, Janecek E, Domecq C, Greenblatt DJ (1981) A method for estimating the probability of adverse drug reactions. Clin Pharmacol Ther 30:239–245
Macedo AF, Marques FB, Ribeiro CF, Teixeira F (2003) Causality assessment of adverse drug reactions: comparison of the results obtained from published decisional algorithms and from the evaluations of an expert panel, according to different levels of imputability. J Clin Pharm Ther 28:137–143
Forster AJ, Clark HD, Menard A, Dupuis N, Chernish R, Chandok N, Khan A, van Walraven C (2004) Adverse events among medical patients after discharge from hospital. Can Med Assoc J 170:345–349
Köhler GI, Bode-Böger SM, Busse R, Hoopmann M, Welte T, Böger RH (2000) Drug–drug interactions in medical patients: effects of in-hospital treatment and relation to multiple drug use. Int J Clin Pharmacol Ther 38:504–513
Bertoli R, Bissig M, Caronzolo D, Odorico M, Pons M, Bernasconi E (2010) Assessment of potential drug–drug interactions at hospital discharge. Swiss Med Wkly 140:w13043. doi:10.4414/smw.2010.13043
Glintborg B, Andersen SE, Dalhoff K (2005) Drug-drug interactions among recently hospitalised patients—frequent but mostly clinically insignificant. Eur J Clin Pharmacol 61:675–681
Obreli Neto PR, Nobili A, Marusic S, Pilger D, Guidoni CM, Baldoni Ade O, Cruciol-Souza JM, Da Cruz AN, Gaeti WP, Cuman RK (2012) Prevalence and predictors of potential drug–drug interactions in the elderly: a cross-sectional study in the Brazilian primary public health system. J Pharm Pharm Sci 15:344–354
Astrand B, Astrand E, Antonov K, Petersson G (2006) Detection of potential drug interactions—a model for a national pharmacy register. Eur J Clin Pharmacol 62:749–756
Obreli-Neto PR, Nobili A, De Lyra Júnior DP, Pilger D, Guidoni CM, Baldoni Ade O, Cruciol-Souza JM, Freitas AL, Tettamanti M, Gaeti WP, Cuman RK (2012) Incidence and predictors of adverse drug reactions caused by drug–drug interactions in elderly outpatients: a prospective cohort study. J Pharm Pharm Sci 15:344–354
Glassman PA, Belperio P, Lanto A, Simon B, Valuck R, Sayers J, Lee M (2007) The utility of adding retrospective medication profiling to computerized provider order entry in an ambulatory care population. J Am Med Inform Assoc 14:424–431
Doucet J, Chassagne P, Trivalle C, Landrin I, Pauty MD, Kadri N, Ménard JF, Bercoff E (1996) Drug–drug interactions related to hospital admissions in older adults: a prospective study of 1000 patients. J Am Geriatr Soc 44:944–948
Lindley CM, Tully MP, Paramsothy V, Tallis RC (1992) Inappropriate medication is a major cause of adverse drug reactions in elderly patients. Age Ageing 21:294–300
Egger SS, Drewe J, Schlienger RG (2003) Potential drug–drug interactions in the medication of medical patients at hospital discharge. Eur J Clin Pharmacol 58:773–778
Bacic-Vrca V, Marusic S, Erdeljic V, Falamic S, Gojo-Tomic N, Rahelic D (2010) The incidence of potential drug–drug interactions in elderly patients with arterial hypertension. Pharm World Sci 32:815–821
Cusack BJ (2004) Pharmacokinetics in older persons. Am J Geriatr Pharmacother 2:274–302
Perazella MA, Mahnensmith RL (1997) Hyperkalemia in the elderly: drugs exacerbate impaired potassium homeostasis. J Gen Intern Med 12:646–656
Uijtendaal EV, Zwart-van Rijkom JE, van Solinge WW, Egberts TC (2011) Frequency of laboratory measurement and hyperkalaemia in hospitalised patients using serum potassium concentration increasing drugs. Eur J Clin Pharmacol 67:933–940
Zwart-van Rijkom JE, Uijtendaal EV, ten Berg MJ, van Solinge WW, Egberts AC (2009) Frequency and nature of drug–drug interactions in a Dutch university hospital. Br J Clin Pharmacol 68:187–193
Iber FL, Murphy PA, Connor ES (1994) Age-related changes in the gastrointestinal system. Effects on drug therapy. Drugs Aging 5:34–48
Madanick RD (2011) Proton pump inhibitor side effects and drug interactions: much ado about nothing? Cleve Clin J Med 78:39–49
Sharma VR, Brannon MA, Carloss EA (2004) Effect of omeprazole on oral iron replacement in patients with iron deficiency anemia. South Med J 97:887–889
Nutescu E, Chuatrisorn I, Hellenbart E (2011) Drug and dietary interactions of warfarin and novel oral anticoagulants: an update. J Thromb Thrombolysis 31:326–343
Cruciol-Souza JM, Thomson JC (2006) A pharmacoepidemiologic study of drug interactions in a Brazilian teaching hospital. Clinics (Sao Paulo) 61:515–520
O’Neill JL, Remington TL (2003) Drug-induced esophageal injuries and dysphagia. Ann Pharmacother 37:1675–1684
Zarowitz BJ (2006) Oral solid potassium chloride and anticholinergic medications: a new drug interaction for an old drug? Geriatr Nurs 27:329–333
McMahon FG, Ryan JR, Akdamar K, Ertan A (1984) Effect of potassium chloride supplements on upper gastrointestinal mucosa. Clin Pharmacol Ther 35:852–855
Newton JL (2005) Effect of age-related changes in gastric physiology on tolerability of medications for older people. Drugs Aging 22:655–661
Siller-Matula JM, Lang I, Christ G, Jilma B (2008) Calcium-channel blockers reduce the antiplatelet effect of clopidogrel. J Am Coll Cardiol 52:1557–1563
Good CW, Steinhubl SR, Brennan DM, Lincoff AM, Topol EJ, Berger PB (2012) Is there a clinically significant interaction between calcium channel antagonists and clopidogrel?: results from the Clopidogrel for the Reduction of Events During Observation (CREDO) trial. Circ Cardiovasc Interv 5:77–81
Fulda TR, Valuck RJ, Vander Zanden J, Parker S, Byrns PJ (2000) Disagreement among drug compendia on inclusion and ratings of drug–drug interactions. Curr Ther Res 61:540–548
Vitry AI (2007) Comparative assessment of four drug interaction compendia. Br J Clin Pharmacol 63:709–714
Abarca J, Malone DC, Armstrong EP, Grizzle AJ, Hansten PD, Van Bergen RC, Lipton RB (2003) Concordance of severity ratings provided in four drug interaction compendia. J Am Pharm Assoc 44:136–141
Vonbach P, Dubied A, Krähenbühl S, Beer JH (2008) Evaluation of frequently used drug interaction screening programs. Pharm World Sci 30:367–374
Barrons R (2004) Evaluation of personal digital assistant software for drug interactions. Am J Health Syst Pharm 61:380–385
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Marusic, S., Bacic-Vrca, V., Obreli Neto, P.R. et al. Actual drug–drug interactions in elderly patients discharged from internal medicine clinic: a prospective observational study. Eur J Clin Pharmacol 69, 1717–1724 (2013). https://doi.org/10.1007/s00228-013-1531-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-013-1531-7